NEWYou can now hear to Fox Information content!
When the finish of the COVID-19 pandemic will come, it could make main disruptions for a cumbersome U.S. well being care program designed more generous, versatile and up-to-date technologically by way of a raft of temporary crisis steps.
Winding down people guidelines could commence as early as the summer time. That could pressure an estimated 15 million Medicaid recipients to uncover new sources of coverage, involve congressional action to preserve wide telehealth access for Medicare enrollees, and scramble specific COVID-19 policies and payment insurance policies for hospitals, medical practitioners and insurers. There are also issues about how crisis use approvals for COVID-19 solutions will be managed.
The array of difficulties is tied to the coronavirus community well being emergency very first declared extra than two decades in the past and periodically renewed given that then. It’s set to stop April 16 and the expectation is that the Biden administration will increase it via mid-July. Some would like a for a longer time off-ramp.
FAUCI: IT May possibly Never BE Distinct Whether or not LOCKDOWNS Had been ‘WORTH IT’ OR ‘TOO SEVERE’
Transitions really do not bode perfectly for the complex U.S. wellness care process, with its blend of personal and authorities insurance and its labyrinth of policies and treatments. Wellness care chaos, if it breaks out, could build midterm election headaches for Democrats and Republicans alike.
“The flexibilities granted by way of the public overall health unexpected emergency have helped persons keep lined and get accessibility to care, so shifting forward the crucial query is how to make on what has been a achievements and not get rid of floor,” mentioned Juliette Cubanski, a Medicare skilled with the nonpartisan Kaiser Household Basis, who has been investigating probable effects of winding down the pandemic unexpected emergency.
MEDICAID CHURN
Medicaid, the condition-federal wellness insurance policies plan for very low-income men and women, is masking about 79 million persons, a history partly thanks to the pandemic.
But the nonpartisan City Institute imagine tank estimates that about 15 million men and women could lose Medicaid when the community wellness unexpected emergency finishes, at a rate of at the very least 1 million per thirty day period.
Congress increased federal Medicaid payments to states for the reason that of COVID-19, but it also necessary states to continue to keep folks on the rolls during the wellbeing crisis. In usual times states routinely disenroll Medicaid recipients whose incomes increase over and above sure concentrations, or for other existence variations impacting eligibility. That method will swap on once more when the crisis finishes, and some states are eager to transfer forward.
Almost all of these getting rid of Medicaid are envisioned to be eligible for some other supply of coverage, both by means of companies, the Cost-effective Treatment Act or — for youngsters — the Children’s Health Coverage Method.
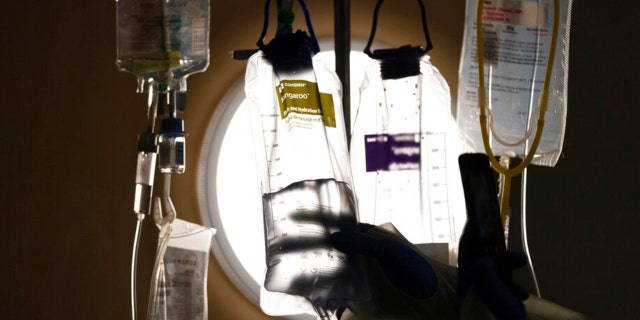
A nurse checks on IV fluids although conversing to a COVID-19 individual at Providence Holy Cross Health-related Heart in Los Angeles, Dec. 13, 2021.
(AP Image/Jae C. Hong, File)
But which is not likely to come about routinely, mentioned Matthew Buettgens, direct researcher on the City Institute review. Expense and absence of consciousness about options could get in the way.
Men and women dropped from Medicaid may possibly not understand they can choose up taxpayer-sponsored ACA coverage. Medicaid is normally no cost, so people made available place of work insurance policy could come across the rates much too superior.
“This is an unprecedented scenario,” explained Buettgens. “The uncertainty is serious.”
The federal Facilities for Medicare and Medicaid Services, or CMS, is advising states to take it slow and link Medicaid recipients who are disenrolled with other probable protection. The agency will keep an eye on states’ accuracy in making eligibility decisions. Biden officers want coverage shifts, not losses.
“We are concentrated generating confident we keep on to the gains in protection we have built less than the Biden-Harris administration,” reported CMS Administrator Chiquita Brooks-LaSure. “We are at the strongest stage in our record and we are heading make sure that we hold on to the coverage gains.”
ACA protection — or “Obamacare” — is an possibility for many who would reduce Medicaid. But it will be much less very affordable if congressional Democrats fail to lengthen generous economical aid known as for in President Joe Biden’s social legislation. Democrats stalling the monthly bill would face blame.
Next COVID BOOSTER SHOT: WHAT TO KNOW
Republicans in primarily Southern states that have refused to expand Medicaid are also susceptible. In people states, it can be very difficult for lower-money grownups to get coverage and much more people could wind up uninsured.
State Medicaid officials really don’t want to be the scapegoats. “Medicaid has finished its work,” explained Matt Salo, head of the Countrywide Affiliation of Medicaid Administrators. “We have appeared out for bodily, psychological and behavioral health and fitness demands. As we arrive out of this emergency, we are meant to right-measurement the system.”
TELEHEALTH STATIC
Hundreds of thousands of People found out telehealth in 2020 when coronavirus shutdowns led to the suspension of schedule health-related consultations. In-man or woman visits are all over again the norm, but telehealth has demonstrated its usefulness and acquired broader acceptance.
The close of the public wellness crisis would jeopardize telehealth obtain for hundreds of thousands enrolled in common Medicare. Restrictions predating COVID-19 restrict telehealth largely to rural residents, in part to mitigate from health and fitness care fraud. Congress has offered by itself 151 times following the close of the general public well being unexpected emergency to appear up with new policies.
“If there are no variations to the legislation soon after that, most Medicare beneficiaries will reduce entry to coverage for telehealth,” the Kaiser Foundation’s Cubanski claimed.
A major exception applies to enrollees in personal Medicare Gain ideas, which generally do address telehealth. However, approximately 6 in 10 Medicare enrollees are in the traditional price-for-support plan.
Checks, VACCINES, Treatments, PAYMENTS & Processes
Widespread entry to COVID-19 vaccines, exams and remedies rests on lawful authority connected to the general public health emergency.
A single example is the Biden administration’s requirement for insurers to deal with up to eight no cost at-property COVID-19 exams for each thirty day period.
An region that’s significantly murky is what transpires to assessments, treatments and vaccines included beneath crisis use authorization from the Food and Drug Administration.
Some authorities say emergency use approvals last only as a result of the length of the general public wellbeing unexpected emergency. Others say it is not as straightforward as that, for the reason that a distinct federal unexpected emergency statute also applies to vaccines, checks and remedies. There’s no clear way nevertheless from health officials.
The Food and drug administration has granted whole acceptance to Pfizer-BioNTech’s COVID-19 vaccine for these 16 and older and Moderna’s for these 18 and more mature, so their ongoing use would not be impacted.
But hospitals could get a financial hit. At the moment they’re compensated 20{fc1509ea675b3874d16a3203a98b9a1bd8da61315181db431b4a7ea1394b614e} additional for the treatment of COVID-19 clients. That extra payment is only for the length of the unexpected emergency.
Simply click Here TO GET THE FOX Information Application
And Medicare enrollees would have much more hoops to jump by means of to be accredited for rehab in a nursing house. A suspended Medicare rule necessitating a prior a few-working day healthcare facility keep would occur again into impact.
Wellness and Human Expert services Secretary Xavier Becerra not too long ago informed The Linked Press that his office is fully commited to supplying “sufficient detect” when it finishes the community wellness crisis.
“We want to make guaranteed we’re not putting in a harmful place Us residents who still will need our help,” Becerra mentioned. “The one particular that persons are genuinely worried about is Medicaid.”