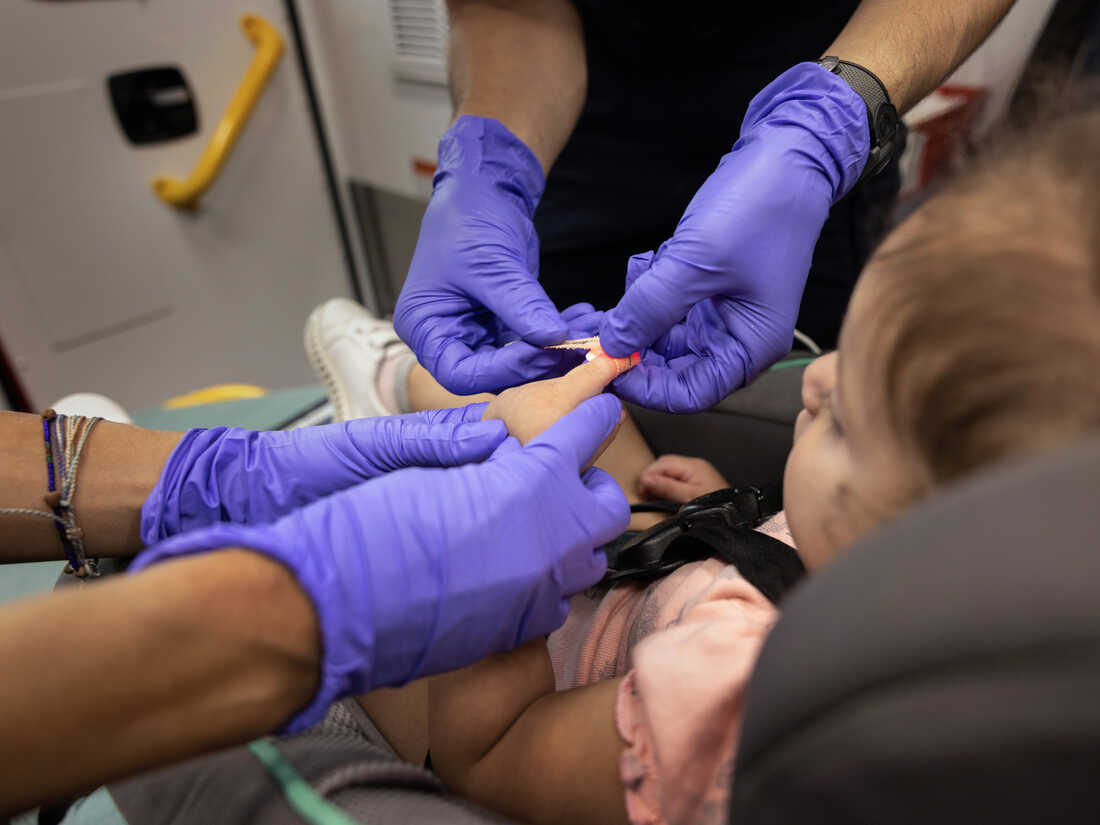
Research shows many hospitals in the U.S. aren’t fully prepared to deal with a surge of sick children.
John Moore/Getty Images
hide caption
toggle caption
John Moore/Getty Images

Research shows many hospitals in the U.S. aren’t fully prepared to deal with a surge of sick children.
John Moore/Getty Images
“Dad, I can’t breathe.”
That’s how Dr. Marc Auerbach’s 8-year-old son woke him up one night last year.
Their family was on vacation in the Adirondack Mountains in upstate New York – hours from Yale New Haven Children’s Hospital, where Auerbach works in pediatric emergency medicine.
Like so many parents whose children have become seriously ill with respiratory syncytial virus (RSV), Auerbach recognized that high-pitched, wheezing sound his son was making. It was a sign his airway was becoming obstructed. He knew they needed to go to the nearest emergency department, right away.
But as Auerbach loaded his son into the car and started driving through the dark mountain roads, he had no idea if the local ED would be fully equipped to treat his child.
“I was quite nervous going in, as a pediatric emergency physician,” he recalled. “Frankly, am I gonna have to treat him myself? Are they even going to have the equipment?”
These days, staff at many children’s hospitals are breathing a sigh of relief. The brutal surge of pediatric illnesses over the fall and early winter – propelled by a tidal wave of common bugs like RSV and influenza – has waned. But for parents who waited hours, or even days, for their child to get a hospital bed, one thing became clear: There just weren’t enough of them.
Even during the best of times, children’s hospitals can find themselves stretched thin, due to years of cutbacks and an ongoing health care staffing shortage. And experts say this latest season exposed what happens to the U.S. health care system when there’s a major crisis of seriously sick children.
“During a surge, when [patient] volumes may double or even more in some communities, that leaves a gap — a major gap,” says Dr. Larry Kociolek, medical director of infection prevention and control at Lurie Children’s Hospital in Chicago. “And children suffer the consequences of that.”
Many EDs are unprepared to care for kids
Auerbach had reason to be wary about taking his kid to an unfamiliar emergency department.
He knew a child’s survival rate is four times higher at an ED that’s well-prepared to care for critically-ill kids. And he knew that too many emergency departments fall short.
In fact, emergency departments receive what’s called a “weighted Pediatric Readiness Score.” It’s a way to assess whether a department has the right equipment, staffing, training policies and patient-safety protocols to care for severely-ill and injured children.
According to a 2015 analysis, the median score is equivalent to a D.
A study published earlier this year, looking at close to 1,000 EDs, found more than 1,400 children’s deaths could have been prevented over a six-year period, if every department had been well-prepared for pediatric cases.
Auerbach stresses that most children do get good care – and parents shouldn’t hesitate to bring their kids in if there is an emergency – but the reality is that children “were not at the focal point ” of the country’s ED system as it developed. In general, EDs treat far more adults than kids.
While children account for 30{fc1509ea675b3874d16a3203a98b9a1bd8da61315181db431b4a7ea1394b614e} of all emergency department visits in the U.S., most of them are seen in EDs that care for fewer than 15 kids per day. That’s why many end up transfering kids to children’s hospitals, which have the resources to treat kids in critical condition, Auerbach says.
But during this most recent wave of illnesses, those specialized hospitals were quickly overwhelmed. “We were seeing that a patient that might require time-critical interventions, was now waiting for those interventions, sometimes six, eight, 12 hours in that community [emergency department] setting,” Auerbach says.


A surge hits after years of cutting pediatric beds
Over the fall and winter, some children’s hospitals doubled-up patient rooms and stretched their limited staff and equipment – all in a desperate attempt not to turn kids away. But they couldn’t undo the years of underinvestment that had whittled away the country’s supply of pediatric beds and trained staff.
Between 2008 and 2018, U.S. hospitals cut nearly 20{fc1509ea675b3874d16a3203a98b9a1bd8da61315181db431b4a7ea1394b614e} of pediatric inpatient units (meaning departments with more than one pediatric bed, such as pediatric intensive care units.) The number of children’s beds dropped by almost 12{fc1509ea675b3874d16a3203a98b9a1bd8da61315181db431b4a7ea1394b614e} – and many of the remaining beds are now concentrated in urban areas, making it even harder for rural families to access care.
Finances – more than anything else – had led hospitals to downsize their pediatric care; hospital beds with children don’t bring in as much money as adult beds do. For example, more than one in three kids are covered by Medicaid. And while Medicaid’s reimbursement rate for hospitals varies widely depending on location, it can often be lower than what hospitals get from caring for an adult who has Medicare or commercial insurance.
“Adult care is often more complex, more chronic, might involve more medications…[and] might be more lucrative,” says Auerbach.
That’s not lost on hospital administrators, Kociolek says.
“That [financial] margin is higher [for hospitals] if you preferentially invest in adult health care,” he says. “So while the adult health care community may benefit from that, the pediatric health care community is left behind.”


How bad will it get next time?
It’s hard to know whether hospitals will see a repeat of this past season anytime soon, says Dr. Kris Bryant, a pediatric infectious disease specialist at Norton Children’s Hospital in Louisville, Kentucky.
“But I suspect all of those viruses will continue to circulate and cause their own surges. And if they all happen at the same time, we will be pressed for beds again,” she says.
Infants are at especially high-risk for severe RSV, but Kociolek says the fact that older kids were also getting really sick put added pressure on the health care system.
“Two- to three-years-old with RSV were doing much worse with that virus than they would have done in 2018 or 2019,” he says.
That could be because those toddlers hadn’t been exposed to RSV and other common viruses after a year or more of social distancing and pandemic precautions, says Bryant. “We had a couple of years in which we didn’t see a lot of respiratory virus circulation.”
So while it’s possible the next fall and winter will look different, Bryant says the health care system needs to take steps now to prepare.
She says getting more kids vaccinated is one way to keep kids out of the hospital. “If we don’t increase the number of kids who are vaccinated, we’ll see outbreaks of vaccine-preventable diseases,” she says, citing the recent measles outbreak in Columbus, Ohio that sickened nearly 100 kids and hospitalized more than 30.
In the meantime, better treatments are also on the horizon: The Food and Drug Administration could approve Pfizer’s RSV vaccine later this year, and other antibody therapies are likely to become more widely available.
But making sure kids can get the best possible care will also require big, systemic changes. “I don’t see how our pediatric health care system can be sustainable without major financial reforms,” Kociolek says. That includes changing how pediatric care is reimbursed, making it more affordable for medical students to choose a career in pediatrics and investing more hospital resources into caring for kids.
In the meantime, community hospitals and smaller emergency departments can essentially serve as “lifeboats” that help out during a storm, Kociolek says. For example, during this past surge, some children’s hospitals used telemedicine to give virtual, round-the-clock assistance to rural or smaller hospitals and EDs.
And emergency departments don’t have to invest in costly specialists or add pediatric beds in order to be better prepared to treat critically-ill and injured children. Most emergency medicine physicians already have some significant training in pediatric care, Auerbach says. Often the biggest improvement comes from designating a staffer to be the pediatric care coordinator — someone whose job is to make sure every aspect of emergency care, from disaster drills to equipment checks, is done with kids in mind.
To Auerbach’s relief, the hospital in rural New York where his son was treated had taken just these kinds of steps. It had partnered with a big university hospital and had the right equipment, the right policies, the right staff training, to handle seriously sick kids.
If every ED was like that, he says, it could save thousands of children’s lives.
“They rapidly assessed him, [and] began very appropriate breathing treatments and medical treatments,” Auerbach says. “And after about six hours of observation, we were able to actually stop at Dunkin Donuts on the way home and come and see his mom and his brother.”
